In the diagnosis and assessment of ME/CFS, there is a great need for simple objective measures that can differentiate the condition from other chronic illnesses, particularly after 24 or 48 hours when the effects of exercise can become most apparent. To date, researchers at Antwerp University Hospital have found upper limb muscle recovery is be slower in ME/CFS patients (read more), and they have also shown that ‘timed-loaded standing’ with a dumbbell (intended to simulate the performance of the torso during everyday activities) is shorter in women with ME/CFS than others, revealing a relative lack of endurance in the muscles of the trunk and arm (read more).
Similarly, an ongoing program of research at Johns Hopkins University has also shown that simple physiological challenges can have abnormal effects. These researchers have uncovered preliminary evidence that ME/CFS patients’ symptoms can be aggravated by ‘neuromuscular strain’, and that young people with the illness have more areas of the body with an ‘abnormal range of motion’ than healthy youngsters. In fact, in the young patients, they found that adding a longitudinal strain to the nerves and soft tissues provoked symptoms, suggesting that the nervous system and connective tissues of the ME/CFS patients is less compliant, i.e. more sensitive to mechanical movement, than normal. Continuing its investigations, the group’s most recent report describes work on 60 people with ME/CFS and 20 controls, who underwent either a real neuromuscular strain for 15 minutes (passive supine straight leg raise or SLR) or a sham leg raise that minimised strain. The SLR, which involves raising and holding up one leg while the person lies on their back on an examination table, is most often used for low-back examinations; in fact, it is a test of nerve root irritation, most often seen in sciatica or lumber disc herniation (read more). In this case, however, it was used only to give a mild to moderate strain to the muscles and nerves.
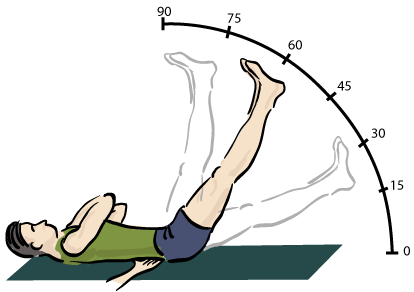
Their most interesting finding was that ME/CFS patients undergoing the SLR, which actually strained their muscles and nerves, had more body pain and concentration difficulties during the procedure than those with the sham leg raise. Not only was the mean composite symptom score significantly greater during the manoeuvre (difference of 3.52 points) in the SLR group than the sham leg raise group, but it was also greater after 24 hours (4.30 points). Also, more patients in the SLR group reported at least a two-point increase in at least three symptoms after 24 hours (44 versus 18%, respectively). As the authors say, “a sustained longitudinal strain applied to the neural and soft tissues of the lower limb was associated with an increased intensity of cardinal symptoms during the manoeuver and for up to 24 hours afterwards”.
They explain the results by pointing to the fact that, in everyday life, the nervous system has to adapt to changes as the body moves, including changes in fibre length and the sliding of nerves within their protective coat of fascia (see a review). Passive SLR exerts a pulling force on a large range of structures (lower limb peripheral nerves, dorsal root ganglia, lumbosacral nerve roots, etc.) and probably gives an elongation strain to the entire length of the spinal cord. Such increased mechanical strain may also cause the spinal blood vessels to narrow, and may stimulate mast cells to release biologically active substances, such as histamine, that worsen both acute and delayed symptoms.
Prof Kevin Fontaine, a co-author of the report, says that the findings “have practical implications for understanding why exercise and the activities of daily living might be capable of provoking CFS symptoms…If simply holding up the leg of someone with CFS to a degree that produces a mild to moderate strain is capable of provoking their symptoms, prolonged or excessive muscle strain beyond the usual range of motion that occurs during daily activities might also produce symptom flares.”
Overall, the results suggest that increased mechanical sensitivity may be a factor in the symptoms people with ME/CFS experience after even mild exertion, and the researchers’ next steps are to tease out the particular effects of strains to muscles and nerves, and to elucidate whether neural or muscular factors predominate. Day-to-day impairments in basic functioning of people with ME/CFS – which can be easily measured objectively in the consulting room, and can be provoked by simple manoeuvres like the SLR – tend to be overlooked by healthcare professionals today, but may well have diagnostic or pathophysiological value.




