We already know that many ME/CFS patients have difficulties standing (orthostasis), particularly standing still (see Standing up for ME). In fact, symptoms of ‘orthostatic intolerance’ can often be found in these patients during clinical assessment (read more) , and there is also evidence that they can have problems walking; for example, one ME Research UK-funded investigation found that the physiological cost of walking was significantly greater for ME/CFS patients than for healthy people, though the reasons for these higher energy demands remain unknown.
Recently, researchers at Antwerp University Hospital have been taking a more in-depth look at the physical capabilities of people with ME/CFS. In one study, they examined upper limb muscle recovery – a feature that had never been subjected to research in ME/CFS, despite the fact that these muscles are most frequently used for everyday activities, such as combing and washing hair, ironing and cooking (read more). After an upper limb exercise challenge, muscle recovery was significantly slower in ME/CFS patients. In another study, they showed that ‘timed-loaded standing’ with a dumbbell (intended to simulate the performance of the torso during everyday activities) was much shorter in women with ME/CFS than in women with osteoporosis or healthy women, revealing a lack of endurance in the muscles of the trunk and arm (read more).
Continuing their programme of work, these Belgian researchers have now examined ‘automaticity’ in women with ME/CFS (read the report). Automaticity involves being able do things ‘automatically’, without the mind being occupied with more basic tasks. For example, the ability to walk and speak at the same time is an example of automaticity; famously, Julius Caesar was able to ride a horse, hold a conversation and read a book at the same time. The facility involves habit, of course; once an activity has been practiced enough, the mind can focus on other activities or thoughts while performing an ‘automatized’ task.
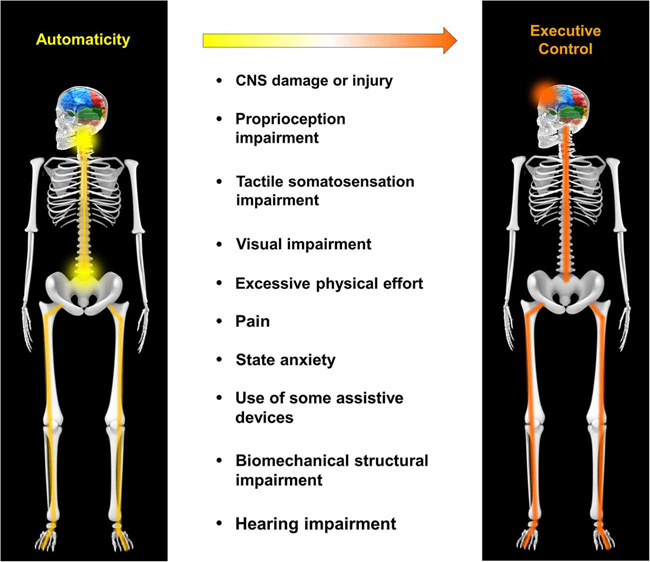
Automaticity while walking (‘gait automaticity’) is no simple task, and a variety of factors can contribute to its impairment, including the central nervous system damage/injury, vision problems, excessive physical effort or pain itself (read more). In modern medical research, assessing gait automaticity is a useful way of assessing frailty and is a good predictor of falls among the frail elderly inside institutions. In ME/CFS, we already know that patients walk far less than healthy people, and that they walk more slowly and at a higher metabolic cost than normal. Also, we know that cognitive performance is impaired in people with ME/CFS, particularly memory and attention (read more), and that sensory ‘overload’ phenomena can be a feature, so it is possible that their cognitive capacity to take on two or more tasks at the same time is reduced.
For this study, the researchers adapted a standard gait automaticity test for use by ME/CFS patients, based on the researchers’ previous observation that ME/CFS patients had difficulties positioning themselves in space when lacking visual data. In the adapted version – the ‘Stops Walking with Eyes Closed with secondary Cognitive Task” (SWECCT) test – patients started to walk with their eyes open (for 7 metres), were then asked to close their eyes and continue walking (for 7 metres), and were then told to continue walking but were asked a simple cognitive question, “How much is 100 minus 7?” Simple enough, you might say, but the results were unexpected.
When starting to walk, only one person out of 38 nondisabled controls (2.6%) looked down at the ground first, whereas eight of the 34 patients (23.5%) checked the floor. After closing their eyes and being asked the question, 19 of the patients (55.9%) found the need to stop walking compared with only 2 (5.3%) of healthy controls. The researchers also observed the ‘deterioration’ in walking at each of these points, i.e. a change in gait less dramatic than stopping, which ranged from mild deterioration (slowing down or extending the arms to keep balance) to severe (losing direction or changing pace dramatically). While walking with closed eyes, 38.2% of ME/CFS patients had either a severe deterioration in their gait or had stopped walking compared with 2.6% of the healthy controls. When the cognitive task was added into the mix, these figures rose to 32 out of 34 (94.1%) of ME/CFS patients compared with just 8 out of 38 (21.1%) controls. Interestingly, the problems ME/CFS patients had with walking and co-ordination was mirrored by a lack of endurance of muscles in arms and trunk, a weakness that the research group in Belgium had previously identified (read their report).
The fact that ME/CFS patients find it a challenge to dual- or multi-task when walking (and, by implication, performing other activities) chimes with findings in patients with other illnesses. We already know, for example, that stroke or Parkinson’s patients and elderly people have a decline in the ability to dual- or multi-task, leading to a deterioration in automaticity and attention. In these groups, the gait becomes more insecure and the risk of falling increases (read a review). Given this, it seems important to ask ME/CFS patients about their experience of falls, either at home or outside; the results may come as a shock to GPs and other healthcare professionals.
Many people with ME/CFS will not be surprised by these results – after all, they have lived for many years with the cognitive impairment and neurological dysfunction that underlie problems with automaticity. And established ME/CFS clinicians have long recognised these symptoms in their patients; as their Canadian Consensus Document said in 2003: “Ataxia, muscle weakness and fasciculations, loss of balance and clumsiness commonly occur. There may be an inability to automatically attune to the environment…and temporary loss of basic habituated motor programs such as walking”. Yet, the day-to-day impairments in basic functioning of people with ME/CFS remain overlooked by the wider clinical and scientific community. To date, in their programme of research, the Belgian researchers have reported a lack of endurance of the muscles in the trunk and arms; a dramatic fall in upper arm strength over a short period; and (in this report) a deterioration in gait automaticity – all of which can yield potentially important clinical information. As we’ve said before, these aspects of everyday living are rarely discussed in the modern literature but may well have clinical or diagnostic value and should not be ignored by medicine today.
Sources
Reduced gait automaticity in female patients with chronic fatigue syndrome: Case-control study. Eyskens JB, et al. J Rehabil Res Dev, 2015; 52(7): 805-14. Read more (full text).
Neurologic aspects and falls. Fasano A & Plotnik M. Clin Cases Miner Bone Metab, 2012 Jan; 9(1): 17-20. Read more (full text).
Timed loaded standing in female chronic fatigue syndrome compared with other populations. Eyskens JB, et al. JRRD, 2015; 52 (1).21-30. Read more (full text).
Recovery of upper limb muscle function in chronic fatigue syndrome with and without fibromyalgia. Ickmans K, et al. Eur J Clin Invest, 2014 Feb; 44(2): 153–9. Read more (abstract).
Automaticity of walking: functional significance, mechanisms, measurement and rehabilitation strategies. Clark DJ. Front. Hum Neurosci, 05 May 2015. Read more (full text).
Automaticity of walking. Clark DJ. Front. Hum Neurosci, 05 May 2015. Read more (full text).



