The fact that ME/CFS has an infectious onset in many cases, and is associated with abnormalities of cellular immunity, raises the question of whether people with the illness are at an increased risk of developing cancer. There is certainly no definitive evidence that this is the case – principally because the large-scale epidemiological studies needed to establish a link have not been conducted. Yet, over the years, there have been intriguing, if inconclusive, hints that there may be an association between ME/CFS and cancer. For example, a survey of deaths from a memorial list in the USA found that one-fifth of the ME/CFS patients listed had died of cancer. And an analysis in 1998 of data from the Nevada Cancer Registry, found the incidence of non-Hodgkin lymphoma and primary brain tumours to be comparatively higher in two northern Nevada counties where well-documented outbreaks of CFS had occurred between 1984 and 1986.
The existence of such fragmentary evidence, plus the biological plausibility that the immune abnormalities or infections found in ME/CFS might increase the cancer risk, led researchers at the National Cancer Institute to undertake a large case–control study (published in Cancer, 2012) among elderly adults in the United States, using linked data from cancer registries and Medicare claims files. The advantage of this experimental design is that very large sample sizes can be obtained, a crucial step if valid conclusions are to be drawn about the connections between highly heterogeneous diseases such as cancer (which contains many different types of tumour at many different stages) and ME/CFS (which is most probably a diagnostic “black box” containing different clinical groups of patients).
The National Cancer Institute’s Surveillance, Epidemiology, and End Results (SEER) program provided the cancer data from registries across the US, with “cases” defined as people aged 66 to 99 years with first cancers from 1992 to 2005. The occurrence of “CFS” was assessed from Medicare claims using ICD codings. For analysis, a combined SEER-Medicare data set was created electronically to allow the link between cancer and ME/CFS to be explored.
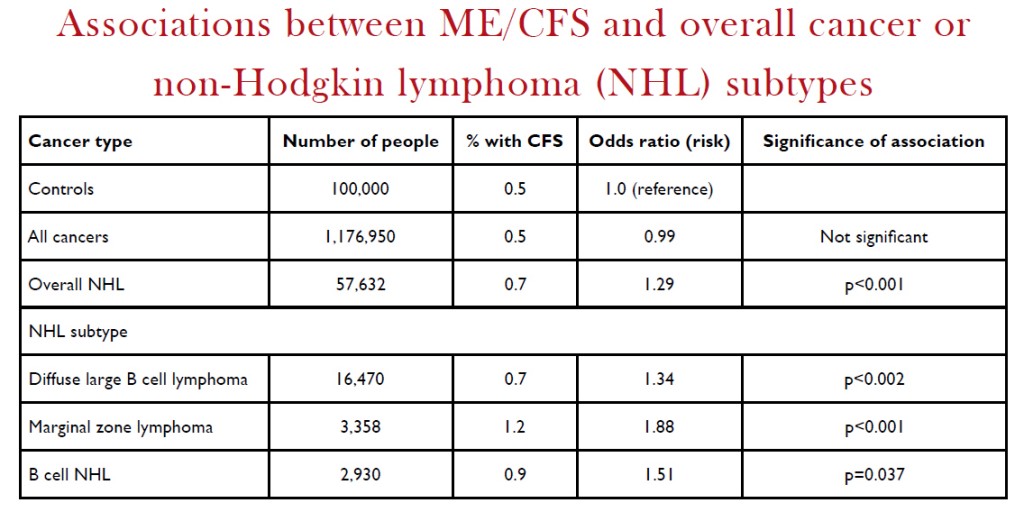
Overall, the presence of CFS was similar in cancer cases and controls (0.5% in each). The table shows that CFS was not associated with cancer overall, but was associated with a significantly increased risk of non-Hodgkin lymphoma (NHL; odds ratio 1.29). Looking at the subtypes of NHL, CFS was associated with diffuse large B cell lymphoma (odds ratio 1.34), marginal zone lymphoma (odds ratio 1.88), and B cell NHL not otherwise specified (odds ratio 1.51). There were also significant associations initially between CFS and a few other cancers, including cancers of the pancreas, kidney, and breast, but these became non-significant after correction for multiple comparisons.
While the finding that the overall cancer risk was not increased is encouraging, what might explain the increased risk of NHL in people diagnosed with CFS in the USA between 1992 and 2005? Well, we can only speculate, but the researchers point to the immune abnormalities (some shared with cancer) that have been observed in ME/CFS patients – including increased immune activation, reduced natural killer cell activity, and the presence of autoantibodies – and to some of the viruses and bacteria that have been implicated in the development and maintenance of the illness. Since both immune disturbances or viral infections have been implicated in the development of diffuse large B cell lymphoma and marginal zone lymphoma in other contexts, the authors suggest that similar associations are at least plausible in ME/CFS. However, they caution that the study was limited to people aged 66 years and older, so that the findings may not be generalisable to younger (non-elderly) populations. Furthermore, they warn against any direct interpretation or application of these results in a clinical setting; as they say, “We could not estimate the absolute risk of non-Hodgkin lymphoma associated with CFS, but the risk is likely too small to affect the clinical management of patients”.